Is the subject of a WCRI webinar at 2 pm eastern TODAY. No charge, but there’s a limit of 500 registrants. Register here.
The webinar follows publication of WCRI’s Dr. Bogdan Savych’s study of Long COVID’s impact on workers’ comp (Study is free to WCRI members; non-members incur a fee).
A very brief summary from WCRI CEO Ramona Tanabe:
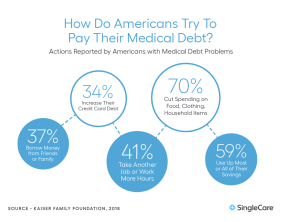
“Among all workers with COVID-19 claims, 6 percent received treatment for long COVID conditions, some more than a year after the initial infection. At an average of 18 months of post-infection experience, these workers received more than 20 weeks of temporary disability benefits and received about $29,000 in medical care.”
Note the relatively low medical cost…$29,000.
Other studies have examined Covid costs for patients covered by commercial health and Medicare Advantage. (note some are NOT Long Covid)
Long Covid – a study published in May of 2022 (note that was a while ago…) indicated the average annual medical costs of LC was $9,000.
CDC – costs average around $9,000 for care in the first 6 months after confirmed infection.
- Using a large electronic administrative discharge database, Shrestha et al estimated a per-patient cost of $24,826 for inpatient care for adult patients with COVID-19.
- Tsai et al examined claims data and found that the mean cost per outpatient visit of a Medicare beneficiary with a COVID-19–related diagnosis was $164.
- Bartsch et al used simulation modeling and estimated median direct medical costs of a COVID-19 diagnosis ranging from $57 to $15,943, depending on the patient’s age and the severity of the case.
- Another study found that COVID-19–related hospital costs per adult hospitalization varied from $8,400 in a general ward to more than $50,000 in an intensive care unit with a ventilator (7).
A useful synopsis of Long Covid issues, treatment, and symptoms is here.
What does this mean for you?
To date, Long Covid is not expensive. Regular readers would have anticipated this.