Drug rebate dollars account for a big chunk of brand drug costs – more than 40% in some cases. While list prices for brand drugs have been rising rapidly, net prices – the prices actually paid to the manufacturer – have not.
That’s mostly because manufacturers have been paying rebates to employers, insurers, and others in the drug distribution system.
This from Adam Fein PhD of Drug Channels:
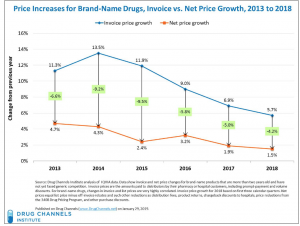
A drug’s net price equals the actual revenues that a manufacturer earns from a drug. The net price equals the list price minus rebates as well as such other reductions as distribution fees, product returns, chargeback discounts to hospitals, price reductions from the 340B Drug Pricing Program, and other purchase discounts.
AARP is one of those making bank off rebates, along with lots of healthplans and insurers.
Workers’ comp
The picture’s a bit different in workers’ comp, for several reasons. Rebate payments tend to be lower because:
- fewer brand drugs are dispensed to work comp patients
- far fewer speciality drugs – the really expensive ones – are dispensed to work comp patients
- the brand drugs dispensed to work comp patients typically don’t have big rebates.
But – there’s always a but – rebates must be considered when evaluating your drug spend. If you are an insurer or self-insured employer, a few things to consider:
- ask your PBM how rebate payments affect your current pricing, and how.
- if you’re pricing a new PBM, ask if you’re going to get the rebates paid directly to you, or if rebates are included in a calculation of your drug price
- find out if you are getting ALL the rebate payments, or other entities in the supply chain are getting a cut. [that’s not necessarily a bad thing, but you do want to know where your dollars are going – because they are your dollars]
- the big PBMs have more buying power, so you’re more likely to get more of the rebate dollars if you’re working with one of the big players
What does this mean for you?
These are your dollars. You need to ask the hard questions to be sure you’re getting the right answers.


