The good.
David Colon and Raji Chadarevian of NCCI have produced an excellent summary of COVID’s impact on workers’ comp medical treatment.
Colleagues Brittni Moore and Vicky Mayen have authored a companion piece that provides an early projection of 2020 financials. While not COVID-centric, there’s no doubt COVID is a main driver of the 8.1% decline in private carrier premiums. Moore and Mayen also note final premium totals may well be lower due to pandemic-driven declines in payroll.
As we projected back in the summer, profits remain robust. The pandemic-driven decline in claims plus carryover from inflated pricing due to the opioid factor are likely chief contributors.
A few takeaways from the COVID study:
- Among COVID claims that had medical expenses, one-fifth had an inpatient stay. Note that this is only for accepted claims WITH medical expenses.
- Among those claims with an inpatient stay, one-fifth – or 4 percent of all claims with medical expenses – were in an ICU at some point.
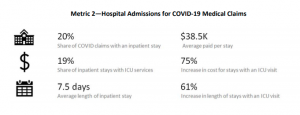
graphic courtesy NCCI
My takeaway – medical costs are relatively low.
Meanwhile Johns Hopkins University researchers studying Accident Fund data report there’s only one industry likely to be significantly impacted by occupational claims for COVID – you guessed it, healthcare.
The highlight – “This suggests that the vast majority of workplaces will not be subject to a high frequency of COVID-19 related WC claims over the course of the pandemic.”
Now, the bad news.
Long Haulers are COVID patients with persistent and often strange symptoms that can persist for month. Possibly related to an immune response gone awry, these conditions include (quoting the NYT):
- fatigue,
- pain,
- shortness of breath,
- light sensitivity,
- exercise intolerance,
- insomnia,
- hearts that race inexplicably,
- diarrhea and cramping, and
- memory problems.
While most patients improve over time, one researcher estimates about one in ten have issues that persist for months.
What does this mean for you?
We have a lot to learn about COVID.



Joe, we do have lot to learn, however; the one thing that should be obvious by now is that we don’t want to get it and we don’t want to transmit it. Further, we have pretty clear evidence as to how we avoid both. Good that we have better leadership stepping in.
Well said – thanks for opining Fred.
be well – Joe
Joe, Following up on Fred’s comment. Here’s an anecdote for those who are post factual regarding Covid data. My daughter is a pediatric resident at a So Cal children’s hospital. The region’s resources are so strained that they are admitting adults into her hospital. For example, she’s taking care of a 55 year old and had a 40 something Covid patient with pulmonary complications in their peds ICU. In giving Covid vaccinations at a stand up clinic recently there is such a sense of relief from the front line care givers as they get their shot. They express how they are relieved for their patients more than for themselves.
Thanks Marc – The willfully ignorant are like drunk drivers, refusing to take responsibility for their actions because they don’t care about other people – or themselves.