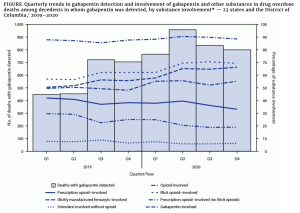
The CDC recently reported gabapentin was involved in one out of every ten fatal overdose deaths in reporting states.
Similar to opioids, gabapentin can cause severe breathing difficulties – which are exacerbated when the drug is combined with other central nervous system depressants (CNS) (e.g. opioids, antidepressants, antianxiety meds).
Illicit use of gabapentin appears to be on the rise…from JAMA:
Gabapentin can produce feelings of euphoria and intoxication and can potentiate opioids’ effects. Individuals who misused the drug reported multiple reasons in a 2019 study, including a desire to enhance the effects of opioids; to achieve a “high” when preferred substances were unavailable, such as when they were living in a treatment facility or were incarcerated; or to self-treat withdrawal or pain. [emphasis added]
Gabapentin is a non-scheduled drug which became much more widely prescribed as opioid scripts declined. Back in 2018 one out of five chronic pain patients were prescribed gabapentin (or its cousin, pregabalin). There’s some evidence that misuse of gabapentin – which is almost always prescribed off-label – often occurs after the consumer had a prescription for the drug.
And, Parke-Davis, manufacturer of Neurontin – the brand name version of gabapentin – pleaded guilty to promoting off-label use and paid a $430 million fine.
So, what to do?
First – learn more. Start here – myMatrixx’ Shanea McKinney, PharmD penned an excellent overview way back in 2019.
Then…
- Dig into your data – what’s been happening with gabapentin?
- When and where possible, require prior authorization for gabapentin and similar drugs.
- Educate patients and caregivers about potential risks of the drug.
- Pay special attention to patients prescribed gabapentin off-label and in combination of other CNS depressants.
- Consider recommending urine drug testing for gabapentin patients and include it in the drug test panel.
What does this mean for you?
This looks awfully familiar.



Gabapentin can be amazingly effective for neuropathic pain but as with literally any medication, needs to be prescribed and used wisely. Let’s be careful and not throw out the baby with the bath water!
Excellent observations Steve – completely agree. It is incumbent on all stakeholders to follow your “prescribe and use wisely” mantra,
be well Joe
Interesting information Joe. Thanks as always. Interesting to note that veterinary medicine use of Gabapentin is on the rise as well. My dog just got a prescription. My vet tells me it is very effective and safer than opioids. Seems the vets are on the same trajectory.
thanks for the note Mark. Coincidentally, our older Newfie is also on gabapentin. cheap as well as effective for her.
be well Joe
Joe – Very timely commentary. Due to concerns over the prescribing of gabapentin in Ohio, effective 11/15/22, pharmacists will be required to check the patient’s record in the state PDMP with each prescription dispensed. The Board of Pharmacy made the change due to the very large increases in prescribing. The PDMP data for 2020 showed the 25% of the patients in the PDMP data base (159,000 patients) received prescriptions for the drug from multiple prescribers. Clearly there has been a shift to this class of medications as the regulatory scrutiny of opioid prescribing has ratcheted up.
thanks as always for the insights John.
As usual Ohio is out in front of this issue; its scary indeed that a quarter of patients with gabapentin scripts got them from multiple prescribers. Hopefully this will be addressed comprehensively and quickly.
be well Joe